In this post, we will be covering on treatment methods for OCD.
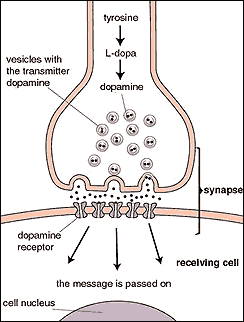
The first type of treatment method is by taking medications. And so what are the medications available for OCD patients? Drugs used for patients suffering from depression are also used for patients with OCD, but in a higher dosage. Selective Serotonin reuptake inhibitors (SSRIs) increase extracellular serotonin levels by inhibiting reuptake, allowing more serotonin to cross the synapse. Selective serotonin reuptake inhibitor (SSRI) drugs such as fluvoxamine, fluoxetine and sertraline are available for OCD patients in Singapore. These drugs have different effects on different people; some may develop side effects but some others might find it completely useful. Psychiatrists may give the patient other drugs, or combine a few of these drugs to a patient who is resistant to a drug (Nobel, n.d.).
The second type of treatment is psychotherapy (NIHM, 2016). Psychotherapy include counselling sessions with a psychiatrist. The only form of psychotherapy that has been proven to be effective in treating this disorder is exposure and response prevention (ERP) (Stanford, 2016). Psychotherapy is an effective way to treat OCD in both adults and children. Around 50% of patients suffering from OCD that undergo this form of treatment benefit from it without the consumption of medications. It is also proven to be effective for those who do not respond well to medication as a form of treatment. 20% to 30% of patients are resistant to this form of treatment. As for patients that underwent psychotherapy for 6 months to three or more years, 25% of them do not benefit much from it. (Stanford, 2016). Psychotherapy can be received at various mental health institutes that provide with a counsellor. Some patients also receive both types of treatment in combination either because just having either treatment is not enough for them or they want to recover at a faster pace.
Apart from having professional help, patients with OCD who are on the route to recovery can join peer support groups to share their experiences. This lets them know that they are not alone in this battle against OCD. Peer support groups such as Sunshinepath run by the Singapore Association of Mental Health (SAMH) allow patients to learn about how others cope with their illness. These groups allows patients to form a tightly-knitted bond with a group of friends which will allow them to gain exposure to social interactions again and they can learn how to integrate back into society once again.
As much as patients require the help of other people who share the same experiences, one of the most crucial players in getting the patients to recover are their family members. As such, groups such as the Caregivers Alliance provides training for caregivers to better understand how they can provide help and support to their family member suffering from OCD.
In Singapore, there is still a stigma around mental illnesses in general. The best way a person struggling with OCD or other mental illnesses could recover is to have support from their loved ones. Mental illnesses are not treated the same as physical illnesses. People need to be aware that mental illnesses do not define a person. With this awareness, people that are struggling with mental illnesses will seek professional help, without the fear of getting judged by the society.