A person with OCD goes through a vicious cycle of obsessive thoughts and compulsive behaviours. These obsessive thoughts are often involuntary, and it can occur in the form of images in their heads (HelpGuide.org, 2016). The compulsive behaviours are done to make the thoughts go away temporarily (HelpGuide.org, 2016). When they get obsessive thoughts, they start to feel anxious. In order to cope with the anxiety, these people act on their thoughts, causing them to behave compulsively. Their compulsive behaviour gives them temporary relief, but not for long.
The exact cause of OCD remains a mystery to scientists. However, scientists believe that a person develops this disorder because of a combination of factors. The factors include neurobiological, environment, cognitive, genetics, and behaviour (UK, n.d.).
We will be covering these factors one by one through our blog posts. In this blogpost, we will be covering the neurobiological factor.
The frontostriatal circuit in our brains are neural pathways which mainly consists of three areas in the brain, the prefrontal cortex, basal ganglia, and thalamus. The prefrontal cortex is in-charge of decision making, the basal ganglia filters information coming from the prefrontal cortex and it is involved in controlling repetitive behaviors. What researchers have found is that basal ganglia can’t properly filter the messages and it ends up sending the wrong signals to the thalamus. Whenever the thalamus receives a wrong signal, it becomes agitated and sends strong signals back to the prefrontal cortex. The prefrontal cortex reacts to these signals by increasing compulsive behavior and anxiety.
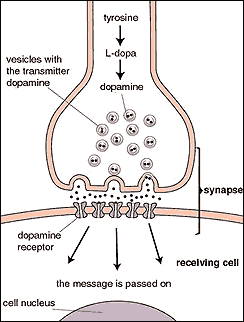
Another part of the neurobiological factor is the imbalance of the neurotransmitter serotonin in the brain. Serotonin helps to regulate mood naturally. It can also help with a couple of body functions like sleeping and digesting. Instead of crossing the synapse, serotonin is reabsorbed back into the nerve cells in the brains of people with OCD. Because of this, vital chemical messages are lost; OCD symptoms develop (Shafagh, 2016).
Very informative and well-explained. Explanations are not too long or complex and is easy to understand. Keep it up!!💪☻
ReplyDelete-Ameera & Atiqah
Hello there, Ameera and Atiqah
DeleteThank you for your comments! We appreciate it! :-)
This comment has been removed by the author.
ReplyDelete